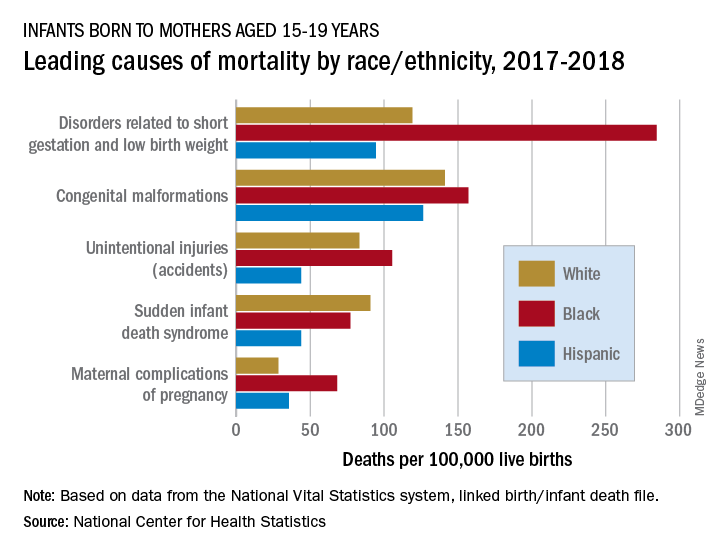
Infant mortality disparity has emerged as a pressing concern in the landscape of healthcare inequality, particularly in the United States. Despite overall advancements in life expectancy for both Black and white Americans, the stark reality remains that Black infants are dying at alarming rates, now twice that of their white counterparts. Recent studies have unveiled that while improvements in mortality rates have been observed, the gap in infant health outcomes continues to widen, revealing a troubling trend of racial health disparities. This issue sheds light on systemic obstacles within the United States healthcare system and underscores the urgent need for strategies to combat infant health inequality. Addressing such disparities not only serves to enhance life expectancy improvement across all demographics but also highlights a critical societal obligation to ensure equitable health for infants irrespective of their race.
The issue of disparities in infant mortality rates has gained significant attention, with many advocating for a deeper understanding of racial healthcare inequalities. Black infant mortality remains a daunting challenge, reflecting broader social and health inequities that disproportionately affect communities of color. This ongoing crisis illustrates a failure in the healthcare system to provide equal care and resources for all infants, leading to unnecessary deaths. Despite advancements in medical practices and policies aimed at improving health outcomes, the persistent gap highlights a critical need for reform. Overall, tackling the issues surrounding racial health inequality is essential for fostering a healthier society where every child has the opportunity to thrive.
Understanding Racial Health Disparities in Infant Mortality
Racial health disparities in the United States, particularly regarding infant mortality, have raised significant concerns over the decades. The most recent study reveals that despite improvements in overall life expectancy for both Black and white Americans, the gap for infants has widened alarmingly. Black infants die at rates that are double those of white infants, reflecting the deep-rooted disparities that permeate the healthcare system. These statistics underscore the urgent need for a comprehensive understanding of the underlying causes of such profound inequalities, which include access to quality healthcare and the socio-economic determinants of health that disproportionately affect Black families.
The widening gap in infant mortality rates exposes a troubling reality—a narrative that healthcare is improving obscures the ongoing crisis faced by Black infants. Medical conditions during pregnancy have been identified as primary contributors to this ongoing disparity, revealing the multifaceted nature of healthcare access and quality. As public health authorities and researchers reflect on these findings, it’s clear that addressing infant health inequality must be a priority. Initiatives aimed at improving access to prenatal care for Black mothers, enhancing healthcare quality, and providing targeted education can be critical steps in reversing these trends.
Factors Contributing to Infant Health Inequality
Infant health inequality stems from a variety of complex factors, including systemic racism within the healthcare system, socio-economic conditions, and lack of access to timely medical care. For Black families, economic disparities can lead to unequal access to quality healthcare services, resulting in higher rates of complications during pregnancy and childbirth. Furthermore, implicit biases within healthcare can affect the quality of care received, leading to situations where Black infants may not receive the same level of attention or care as their white counterparts. The need for systemic change is paramount to ensure that all infants, regardless of race, have equal opportunities for survival and healthy development.
Moreover, public policy must focus on addressing these disparities to create a more equitable healthcare infrastructure. This includes investing in community health programs that empower Black mothers and families, enhancing educational resources surrounding prenatal and infant care, and ensuring that healthcare professionals receive training to mitigate unconscious bias. By identifying and addressing these systemic issues, the United States can work towards closing the gap in infant mortality rates and improving overall health outcomes for Black infants.
Implications of Differential Mortality Rates for Public Policy
The alarming statistics surrounding Black infant mortality should serve as a decisive wake-up call for public policy and public health advocates. The study underscores that if Black Americans had access to the same healthcare resources and quality of care as white Americans, it is estimated that approximately 5 million lives could have been saved in the past 70 years. This staggering figure not only highlights the critical health disparities but also calls into question the adequacy of current policies aimed at reducing racial health differences. Policymakers must prioritize equity in health access to address these urgent disparities, focusing not only on treatment but also on the prevention of health problems.
In response to these findings, public health authorities should implement policy changes that ensure equitable resources for maternal and infant health. This could include expanding Medicaid coverage for expectant mothers, incentivizing healthcare providers to practice in underserved communities, and establishing partnerships with local organizations to support high-risk families. By integrating a robust, equity-focused approach in healthcare legislation, we can begin to bridge the health gap that has persisted for decades and work towards a future where all infants, regardless of their racial background, have equal chances at survival and thriving.
Historical Context: The Journey of Life Expectancy Improvements
Over the last 70 years, life expectancy has improved significantly for both Black and white Americans, with notable gains highlighting advancements in medicine and public health. However, the historical context of these improvements cannot be ignored, especially when one considers the disparities that continue to persist—particularly for Black infants. The trajectory of life expectancy improvement has been positive, yet it remains misleading without acknowledging the areas where significant gaps still exist, specifically in infant mortality rates. While adults see benefits from these advancements, the alarming trend of increasing mortality among Black infants indicates these improvements do not uniformly benefit all racial groups.
Understanding this historical context is crucial for addressing ongoing disparities. The progress made must be tempered with an honest assessment of who has benefited from these advancements. As health policies evolve, it is imperative to integrate lessons learned from the past, ensuring that future public health initiatives do not neglect the unique challenges faced by marginalized communities. This approach can facilitate a more equitable healthcare system that recognizes, addresses, and ultimately works to diminish the systemic inequalities impacting infant health.
The Role of Research in Highlighting Racial Disparities
Research plays a pivotal role in illuminating the racial disparities that exist within the healthcare system, particularly regarding infant mortality rates. The comprehensive analysis conducted over the past seven decades has revealed critical information that previous studies on shorter time spans may have overlooked. This long-term perspective is essential in recognizing the persistent challenges faced by Black infants and understanding how healthcare inequalities have evolved. By amplifying these findings, researchers can inform policymakers and health officials about the urgent need to direct resources and attention to these discrepancies.
Moreover, continuous research is necessary to explore the underlying causes contributing to racial health disparities. It is vital for academic institutions and health organizations to collaborate on studying the factors that disproportionately affect Black infants, including socio-economic conditions, geographic barriers to care, and institutional biases within healthcare. The results of such research can drive effective interventions, spearhead awareness campaigns, and ultimately lead to systemic changes that improve healthcare outcomes for all infants—highlighting that research is not just an academic exercise but a crucial tool for social equity.
Community Interventions: Addressing Infant Mortality at the Local Level
Local community interventions can play a transformative role in addressing the disparities that fuel infant mortality rates. Grassroots initiatives tailored specifically to the needs of Black families can help bridge the significant gaps that current healthcare systems often overlook. These programs may include educational workshops about prenatal care, access to lactation consultants, and family support groups that focus on health during and after pregnancy. By fostering community engagement and support, these initiatives can empower families with knowledge and resources that promote healthier outcomes for infants.
Additionally, local healthcare providers can work alongside community organizations to create culturally competent care models that recognize and respect the backgrounds and experiences of Black families. Ensuring that caregivers understand cultural nuances can improve trust and ultimately the quality of care provided. Community-based interventions not only address immediate health needs but also foster a collaborative environment that holistically supports families in their journey towards healthier infant outcomes. By prioritizing community involvement, we can take significant steps towards reducing the shocking disparities in infant mortality.
Legal and Ethical Considerations in Healthcare Disparities
The legal and ethical implications of healthcare disparities, particularly in infant mortality, cannot be overlooked. There is a growing recognition that every individual has fundamental rights to equitable healthcare services. When systemic racial disparities permeate healthcare systems—resulting in different outcomes based on race—this raises profound ethical questions about fairness and justice in public health. Advocates for equitable healthcare argue that addressing these disparities is not just a matter of improving healthcare access; it is a moral imperative that demands attention and action from both the legal and medical communities.
Furthermore, legal frameworks may need to evolve to better address racial inequalities in infant mortality rates. This could involve updating health policies to include stricter regulations against discriminatory practices in healthcare settings, as well as implementing laws that mandate equity assessments for all healthcare initiatives. By intertwining ethical considerations with legal accountability, there lies potential for creating a healthcare system that serves all individuals with the respect and care they rightfully deserve. Ensuring that infant healthcare is free from the shackles of racial disparities will be pivotal in moving toward a more equitable future.
Long-Term Solutions for Reducing Infant Mortality Disparities
While awareness of infant mortality disparities is a vital first step, it is crucial to implement long-term solutions that effectively address these issues. These solutions should not only focus on immediate healthcare access but also tackle the broader socio-economic factors that contribute to health inequities. Policymakers must consider integrated approaches that improve maternal health, provide economic support to at-risk families, and improve education regarding available healthcare resources. Investing in these areas will create a more supportive environment for mothers and infants, ultimately leading to healthier outcomes.
Additionally, sustained funding and commitment from both government and private sectors are necessary to support innovative programs designed to mitigate these disparities over the long term. This could include initiatives aimed at enhancing mental health services for mothers, community health worker programs that provide personalized support, and partnerships with local organizations to create a robust support network. By focusing on strategic, long-lasting solutions that bridge the healthcare divide, it is possible to make meaningful progress in reducing infant mortality rates and ensuring that all infants have an opportunity to thrive.
Frequently Asked Questions
What is the current status of Black infant mortality disparity in the United States?
The Black infant mortality disparity in the United States is alarming, as Black infants die at twice the rate of white infants. While overall mortality rates between Black and white Americans have improved, the gap for infants has actually widened, increasing by 115 percent since the 1950s.
What factors contribute to racial health disparities in infant mortality?
Racial health disparities in infant mortality are caused by a combination of factors, including healthcare access inequality, differences in the quality of care received, and medical conditions during pregnancy. These multidimensional issues impact Black infants disproportionately, leading to higher mortality rates.
How has life expectancy improvement affected Black infant mortality rates?
While life expectancy improvement has generally increased for both Black and white Americans, it has not translated to reduced Black infant mortality rates, which have worsened over the decades. This indicates systemic healthcare inequalities that persist despite advancements in overall life expectancy.
What are the implications of identifying infant health inequality in the United States?
Identifying infant health inequality in the United States underscores the urgent need for targeted public health policies that address systemic disparities. Recognizing the factors contributing to Black infant mortality can inform strategies for improving care and ensuring equity in healthcare resources.
What can be done to address the widening gap in Black infant mortality rates?
To address the widening gap in Black infant mortality rates, policymakers must prioritize access to quality maternal and infant healthcare. Initiatives could include expanding healthcare coverage, improving prenatal care for Black mothers, and addressing social determinants of health that disproportionately affect marginalized communities.
What does the recent study reveal about trends in racial disparities in infant mortality?
The recent study indicates that, despite some improvements in life expectancy, racial disparities in infant mortality rates have not only persisted but worsened. This finding serves as a crucial indicator of ongoing inequities in healthcare access and quality in the United States.
How significant is the difference in healthcare outcomes between Black and white infants?
The significance of the difference in healthcare outcomes is stark, with Black infants experiencing mortality rates 115 percent higher than white infants. This stark contrast highlights the persistent and troubling infant mortality disparity rooted in systemic racial health inequalities.
| Key Points |
|---|
| Americans’ life expectancy has increased over the last 70 years, but disparities persist between Black and white populations. |
| Mortality rates for infants show a significant widening gap; Black infants die at twice the rate of white infants. |
| Black life expectancy improved from 60.5 years in the 1950s to 76 years in the 2010s, a 20.4% increase, while white life expectancy rose from 69 to 79.3 years, a 13% increase. |
| The infant mortality gap has increased from 92% in the 1950s to 115% today. |
| Medical conditions during pregnancy are identified as the leading cause of excess deaths among Black infants in recent years. |
Summary
Infant mortality disparity continues to be a pressing issue in the United States. Despite overall improvements in health outcomes and life expectancy for both Black and white Americans since the 1950s, the alarming fact remains that Black infants are still dying at significantly higher rates than their white counterparts. This widening gap highlights systemic healthcare inequalities that demand immediate attention from policymakers and public health leaders. Understanding the root causes and implementing effective interventions are crucial steps needed to eradicate the disparities in infant mortality rates and ultimately ensure equitable health for all children.